It’s a breathing fact that there are differences in breathing capacity between the sexes. For instance, females have disproportionately smaller radial rib cage dimensions and shorter diaphragm compared to males, making it harder to move air in and out of the lungs. But it’s not only this that affects the amount of lung capacity we have, but age, body composition and ethnicity are factors too.
At rest, an adult will generally breathe around 12-20 times a minute. This equates to just a few litres of air moving in and out of your lungs. However, during vigorous exercise this can raise to around 100 litres per minute.
Breathing Facts
- Expiration is normally passive (only during heavy exercise workloads does it become forced).
- Inspiratory muscles play a vital role in the efficiency of breathing at rest and also during exercise.
- Strength of the inspiratory muscles reduces with age (approximately age 25 years).
- Weaker inspiratory muscles are usually highlighted with breathlessness, especially in the elderly.
- At rest we use as little as 8-12 litres of air per minute.
- During exercise we can use around 100 litres of air per minute. Elite male athletes may even use twice this amount.
- Respiratory rate is a significant predictor of critical illness.
Breathing And Exercise
A study shows that your breathing muscles can contribute to limiting your performance. If, during high intensity exercise, you push your breathing to its limit, then you are exercising above your lactate threshold. It is at such exercise intensity that your breathing rate increases and moves out of its ‘comfort zone’. You will perceive this sudden increase in inspiratory muscle work as breathlessness.
At low and moderate exercise intensities, breathing is very modest. However, as the intensity becomes more strenuous, breathing increases becoming almost exponential.
During the majority of your everyday activities, your breathing operates well within its ‘comfort zone’. Only when you venture above your lactate threshold will you stimulate your breathing sufficiently to challenge your breathing muscles.
Exercising above your lactate threshold is usually short in duration. This means there is not a training stimulus of sufficient duration and frequency for your breathing muscles to experience adaptation. It’s also doubtful whether this type of unloaded breathing will provide an adequate training overload to elicit maximal training benefits. To illustrate this, think how ineffective a bicep curl would be without a weighted dumbbell to overload the muscle with.
This is not to say that aerobic activity doesn’t provide any training benefit to your inspiratory muscles; it does, it’s just not sufficient to elicit the full potential of this vital group of muscles. The result is that under normal conditions, your breathing muscles will never really get trained to cope with ‘heavy breathing’. This is why breathing will always present an uncomfortable challenge. However, with POWERbreathe Inspiratory Muscle Training, you can subject your breathing muscles to a sufficient stimulus that will elicit improvement in breathing muscle strength and stamina, and consequently, a reduction in breathing fatigue.
How Breathing During Exercise Affects Other Muscles In The Body
Research evidence suggests that during heavy exercise, blood flow (and hence oxygen delivery) to the exercising legs is inversely related to respiratory work. What this tells us is that the inspiratory muscles are capable of stealing blood from other working muscles. As a result, performance is impaired. But there is something you can do about it. You can train your breathing system separately to improve your inspiratory muscle strength and stamina.
Breathlessness In Unfit And Fit People Alike
Breathlessness is a common feature of lung and heart disease, as well as, a feature of normal exercise. Research shows that the strength of your inspiratory muscles has a direct influence on how hard you breathe. It also influences how breathless you may feel whilst doing it.
If your inspiratory muscles are weak or fatigued (they can fatigue by as much as 20%) then you’re not able to breathe as hard and your breathing will require greater effort. You feel this as being breathless.
It’s a feeling not dissimilar to how much heavier a dumbbell will feel on an 8th bicep curl than it did on the first. So, if your inspiratory muscles are feeling weak or tired, your breathing will feel harder.
How The Inspiratory Muscles Contribute To The Breathing Process
What happens when you breathe is your diaphragm and chest wall muscles act together like a bellows to pump air in and out. To breathe in your inspiratory muscles contract to expand your chest cavity which causes a pressure drop into which air flows. In fact, it is your inspiratory muscles that undertake most of the work of breathing. To breathe out, you simply relax and air is forced out of your lungs. During exercise the contraction of your abdominal muscles assist with your exhalation.
Causes Of Inspiratory Muscle Weakness
Weakness of the inspiratory muscles can result from a number of causes, including disease, but a potent influence upon their condition is the amount of exercise they receive. The phrase ‘use it or lose it’ applies equally well to the inspiratory muscles as it does to your leg muscles. If you get out of breath on the stairs, then you’ll take the lift, with the consequence that your inspiratory muscles get less exercise.
As your breathing muscles become weaker, the level of physical activity that brings on breathlessness gets lower, so you avoid the stairs even more. It’s a vicious cycle of breathlessness, lack of exercise and inspiratory muscle weakness. In addition, the use of oral steroid medication (not inhaled steroids) to control lung inflammation in conditions such as asthma and emphysema is shown to cause inspiratory muscle weakness. (Inhaled steroids do not cause inspiratory muscle weakness.) This inspiratory weakness can impair lung function and can be counteracted by inspiratory muscle training.
Breathing Fact
By applying the same, simple exercise principle of “USE IT or LOSE IT” to your inspiratory muscles, you will increase your performance.
Facts About Expiratory Muscle Training
There is evidence that expiratory muscle training improves maximal expiratory pressure (MEP) in certain conditions. MEP reflects the strength of your abdominal muscles and other expiratory muscles and is an indicator of respiratory weakness. Forced expiration, such as during exercise or coughing, requires your abdominal muscles to force your diaphragm upward, so strengthening them with expiratory muscle training (EMT) to improve MEP is beneficial.
However, two studies in healthy people that implemented simultaneous Inspiratory Muscle Training (IMT) and Expiratory Muscle Training (EMT) within the same breath cycle, found that this concurrent training actually impaired training responses. Therefore, there is a strong argument for the use of expiratory and inspiratory muscle training to be performed independently of each other.
- A carefully conducted study on rowers found that during combined inspiratory and expiratory muscle training, the expiratory training impairs the effects of inspiratory training.
- A study of inhale/exhale training in swimmers found that combining inhale/exhale training at the same time is less effective than inspiratory training alone.
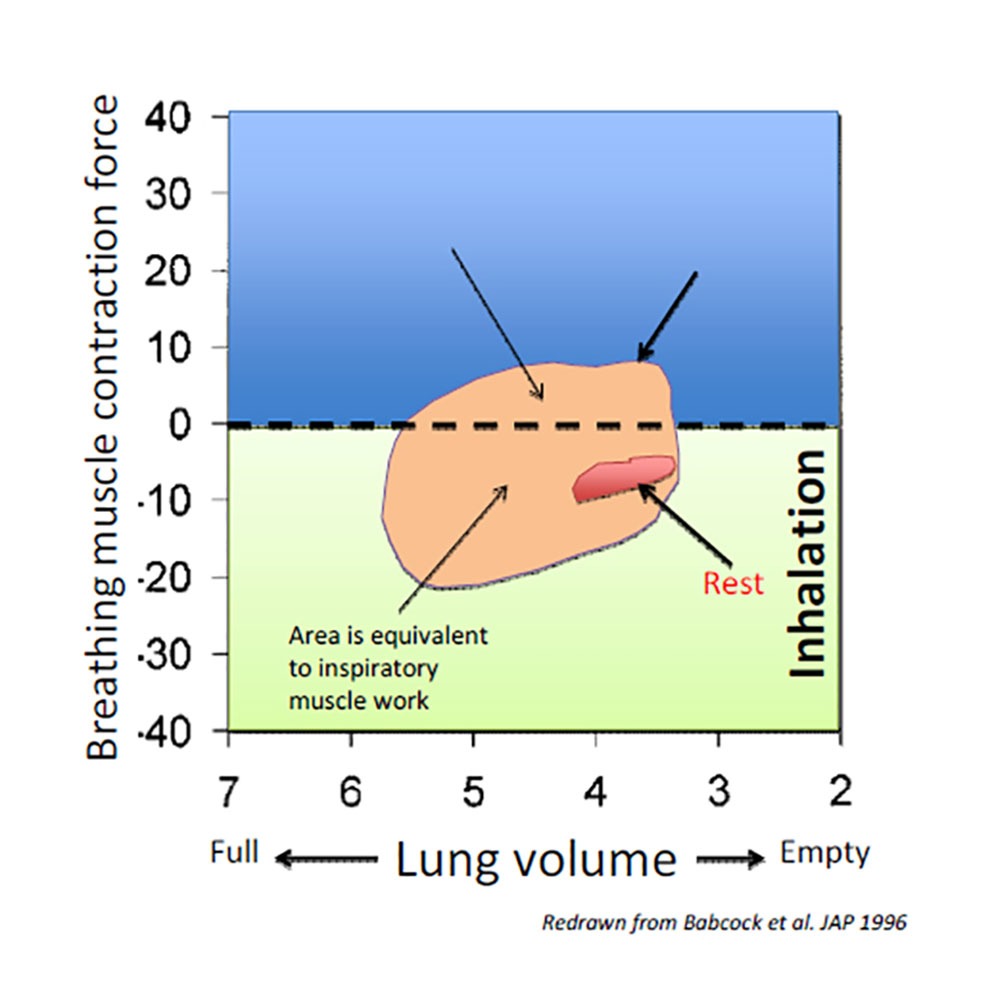
Figure 1 shows changes in breathing muscle contraction force and the resulting changes in lung volume at rest (red loop) and exercise (orange loop). The area below the dashed line represents the amount on inspiratory muscle work. The area above the dashed line shows the amount of expiratory muscle work.
During exercise it is also clear that inspiratory muscle work is much higher than expiratory muscle work (as represented by the amount of orange in the green area compared with the amount in blue). Finally, it’s also worth noting that at rest, all breathing muscle work is inspiratory.






